Many rehab programs build strong gait training sessions, then lose momentum during transition to real walking. That gap slows progress, frustrates therapists, and leaves patients between device categories.
A hip exoskeleton is a wearable hip assist device that supports walking during the transition phase between intensive gait training and more independent mobility. In rehabilitation, it can help selected patients practice corridor walking with less effort and more confidence under professional supervision.

I think this category deserves much more attention than it usually gets. In many departments, the big technology conversation starts with a Gait Training Exoskeleton. Then it jumps straight to discharge planning. But there is often a missing middle step. That step is where the Hip Assist Exoskeleton can make sense. If your team wants to build a more complete lower-limb rehab pathway, keep reading. This is often the device that connects the training room to the corridor and, later, to the community.
What Happens After Intensive Gait Training?
Many patients improve inside structured gait sessions, but that does not mean they are ready for daily walking demands. This creates a transition gap that many rehab pathways do not address well.
After intensive gait training, some patients still need lighter, more mobile walking support before they can manage corridor ambulation or community-oriented practice. This transition phase gait rehab stage often sits between high-support robotic training and independent walking.

I hear this from physiotherapists again and again. A patient can perform well during a guided session, but the next step is less clear. The large gait trainer may be too much for corridor practice. A simple aid may be too little. That mismatch creates the gap.
Why the gap matters
A structured gait trainer gives support, repetition, and safety during intensive practice. But real rehabilitation does not end there. Patients still need to move through hospital corridors, longer walking routes, turning tasks, and more variable daily movement situations.
This stage often exposes a problem. The patient has gained basic walking ability, but still lacks enough hip drive, step consistency, or endurance for practical mobility. The therapist then has to bridge that gap with manual cueing, close supervision, and repeated short-distance walking practice.
Why this stage is often overlooked
Many equipment plans focus on early-stage standing and gait restoration. Discharge planning then focuses on simple mobility aids. The middle phase receives less equipment attention because it looks less dramatic. But from a pathway design view, it is critical.
In one patient pathway review, the rehab team mapped each stage from early standing to discharge. At first, the focus stayed on the obvious milestones. Everyone talked about the first standing sessions, the formal gait trainer block, and the final discharge plan with simple mobility aids.
But when we looked more closely at the pathway, we saw the biggest drop-off happened after the formal gait trainer sessions ended. Patients often left the structured support of the larger system, but they were still not stable enough for efficient corridor walking with minimal assistance.
That middle phase had less equipment attention because it looked less dramatic than first standing or first walking. But the therapists told us it created real workflow pressure. Patients still needed repeated walking practice, but the available tools did not always match that need well.
That review changed the discussion. The team stopped seeing the middle phase as a short transition and started treating it as a critical part of the rehabilitation pathway.
What this means for pathway design
If a department wants continuity, it needs tools for more than one rehab stage. A complete lower-limb pathway should include early intensive gait training, transition-phase walking support, and later-stage daily mobility support where appropriate. That is why I see the Hip Assist Exoskeleton as a practical bridge, not a niche add-on.
What Do Hip Exoskeletons Actually Do?
Some people hear “hip exoskeleton” and imagine a smaller version of a full gait trainer. That is not the right way to understand the category.
A Hip Assist Exoskeleton supports hip movement during walking, especially hip flexion and related gait initiation tasks. It is designed to assist selected patients during transition-phase mobility practice, not to replace intensive robotic gait training.

The simplest way to describe the device is this. It helps the patient move the legs forward more easily during walking. That support can matter a great deal in the transition phase.
Assisted hip flexion
Hip flexion plays a central role in step initiation and swing. After stroke or in geriatric deconditioning, patients may struggle to bring the leg forward with enough timing and confidence. A hip assist device can provide powered support at the hip to reduce that effort.
Corridor walking support
This is where the category becomes very practical. A Hip Assist Exoskeleton can support walking outside the fixed training station. It can help selected patients practice corridor walking, turning, and repeated ward-level ambulation under professional supervision.
Mobility support with less hardware burden
Compared with a larger Gait Training Exoskeleton, a hip exoskeleton is usually lighter and less restrictive. That does not make it better in all cases. It makes it better suited for a different stage.
| Device category | Main role | Typical rehab stage | Typical environment |
|---|---|---|---|
| Gait Training Exoskeleton | Intensive guided gait practice | Earlier or heavier-support stage | Therapy room |
| Hip Assist Exoskeleton | Transition-phase walking assistance | Mid-stage walking progression | Corridor, ward, supervised walking route |
| Ankle Assist & AFO Solutions | Distal support and foot clearance help | Later-stage or targeted gait deficits | Clinic, ward, selected daily mobility settings |
What therapists often notice
Clinical feedback often focuses on smoother step initiation, more repeatable corridor walking, and lower therapist burden during walking supervision. I use careful language here because individual results depend on patient profile and clinical protocol under professional supervision.
Which Patients Fit a Hip Exoskeleton Best?
Hospitals often ask whether this device suits broad rehab populations. The honest answer is no. It suits specific transition-phase profiles.
Hip exoskeleton rehabilitation often fits selected post-stroke patients, transition-phase walkers, and some geriatric cases who need mobile hip assistance but not a full gait trainer. Patient selection depends on strength, balance, cognition, endurance, and therapy goals.

I always encourage teams to think in terms of function first. Diagnosis matters, but walking status matters more.
Post-stroke patients
This is often the clearest group. A post-stroke patient may leave intensive gait sessions with enough standing and stepping ability to start walking beyond the therapy room, but still show limited hip advancement, asymmetry, or fatigue. In that case, a hip assist device stroke pathway may be worth evaluating.
Transition-phase neurological patients
This includes patients who no longer need full robotic guidance, but still need wearable assistance to keep gait practice active and safe.
Geriatric rehabilitation
Some geriatric patients may also fit, especially when deconditioning, low step quality, or reduced endurance slows the move toward practical walking. These cases require very careful selection and therapist oversight.
Basic screening questions
| Selection question | Why it matters |
|---|---|
| Can the patient tolerate upright walking practice? | Safety comes first |
| Does the patient need targeted hip support rather than full-leg guidance? | Clarifies device role |
| Can the patient follow therapist cues? | Supports safe use |
| Is corridor walking a current rehab goal? | Aligns treatment with device value |
| Will a lighter wearable improve workflow over a larger system? | Supports pathway efficiency |
I remember a post-stroke case discussion that made this point very clear.
The patient had improved beyond the stage of needing a full gait trainer for every session. The team felt encouraged by that progress. But the same patient was not ready for unsupported corridor walking either.
The therapists described a gap. The patient could tolerate upright walking practice and could follow cues, but still needed targeted hip support and a more practical way to train walking in real ward spaces.
That changed the device discussion. Instead of asking whether the patient still needed a full gait trainer, the team asked what level of support would help the next stage of recovery.
A lighter wearable option made more sense for that point in the pathway. It matched the patient’s current function better and helped the therapists continue task-based walking practice without moving back to a larger system.
How Does Hip Assist Fit Between the Gait Trainer and Discharge?
Many rehab teams know the two ends of the pathway well. They know intensive training. They know discharge planning. The bridge between them is less structured.
A Hip Assist Exoskeleton fits between the Gait Training Exoskeleton and discharge by supporting supervised walking progression in a more mobile, real-world ward context. It can help departments create a smoother clinical workflow during the transition phase.
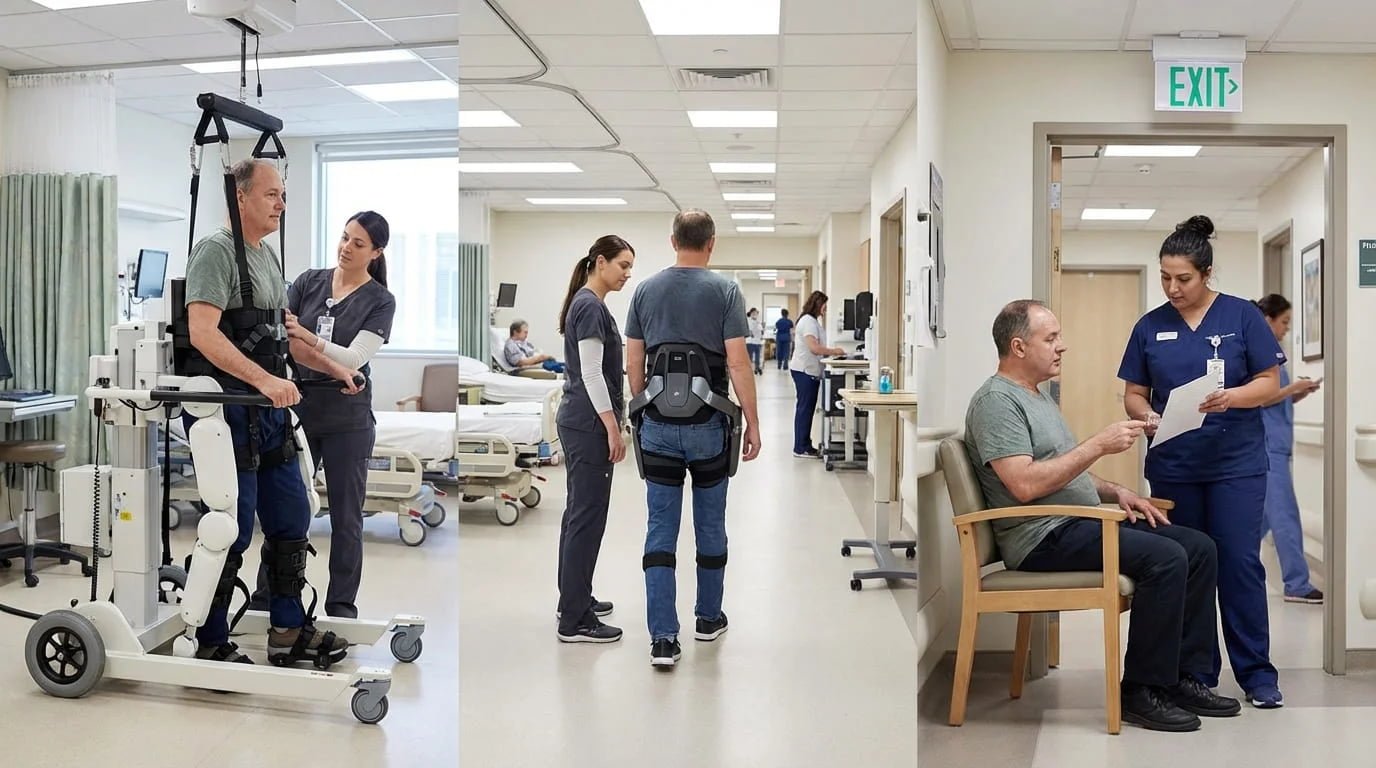
When I map pathways with hospitals, I often draw three stages instead of one long line. That simple change helps teams see where a hip exoskeleton can add value.
Stage 1: Intensive gait training
The patient starts with higher-support walking work. A Gait Training Exoskeleton or another structured system supports repetition, stepping practice, and therapist control.
Stage 2: Transition-phase walking
The patient begins moving beyond the fixed training area. The therapist wants more corridor walking, practical turning, and repeated supervised ambulation. This is where the Hip Assist Exoskeleton often fits best.
Stage 3: Discharge-oriented mobility
The patient moves toward simpler support tools, home planning, community goals, or longer-term mobility aids as appropriate.
Example workflow table
| Rehab stage | Main clinical goal | Device type often used |
|---|---|---|
| Intensive training | Build repetitive gait capacity | Gait Training Exoskeleton |
| Transition phase | Support mobile supervised walking | Hip Assist Exoskeleton |
| Discharge preparation | Prepare for practical daily mobility | Simpler aids or targeted support tools |
This pathway view also helps purchasing committees. Instead of asking whether one machine can do everything, they can ask which missing stage needs support most.
What Should You Check Before Choosing a Hip Exoskeleton?
Not every hip assist device fits clinical rehab well. Some products look attractive on paper but fail during daily use because setup, comfort, or control is weak.
Key selection criteria include device weight, donning time, control modes, comfort, adjustability, and how well the device fits your workflow. In transition phase gait rehab, ease of use often matters as much as technical power.

I think buyers should spend less time on brochure language and more time on therapist questions. If a device is too heavy, too slow to fit, or hard to tolerate, it will not become part of routine practice.
Weight
A lighter device usually supports better therapist acceptance and easier patient use. Weight affects fatigue, confidence, and setup practicality.
Donning time
If setup takes too long, therapists will avoid the device during busy schedules. I always ask teams to measure real donning and doffing time during demos, not ideal vendor timing.
Control modes
Different patients need different levels of assistance. A useful hip assist system should offer clear, usable control options that clinicians can understand without engineering support.
Comfort and fit
Padding, strap design, movement freedom, and noise all affect whether the patient accepts the device. Comfort is not a small detail. It is a use decision.
Workflow compatibility
The best device is the one that fits daily rehab operations. That includes charging, cleaning, transfer handling, and storage.
| Selection criterion | What to evaluate during demo |
|---|---|
| Weight | Can the patient and therapist manage it comfortably? |
| Donning time | How many minutes does setup take in real use? |
| Control modes | Are settings easy for clinicians to understand? |
| Comfort | Does the patient tolerate a full session well? |
| Adjustability | Can the team fit different body types? |
| Workflow fit | Does it slow or support the normal therapy routine? |
What Are the Most Common Misconceptions About Hip Assist Devices?
A device in the middle of the pathway often gets misunderstood. That confusion can block adoption.
The biggest misconception is that a hip assist device should replace a gait trainer. It should not. A Hip Assist Exoskeleton fills a different rehab role and works best when the team understands its limits.

I see four misconceptions most often.
Misconception 1: It is just a smaller gait trainer
It is not. A Gait Training Exoskeleton focuses on structured gait rehabilitation with more support and control. A Hip Assist Exoskeleton supports mobile walking progression.
Misconception 2: It works for everyone who walks slowly
It does not. Slow walking alone is not enough reason. The patient must need hip-focused assistance and fit the safety profile.
Misconception 3: It replaces therapist supervision
It does not. The device still requires professional supervision, patient selection, and progression control. Individual results depend on patient profile and clinical protocol.
Misconception 4: It is mainly a home-use consumer product
That framing misses the rehab value. In this article, I am discussing clinical pathway use inside professional rehabilitation settings, especially during transition-phase gait rehab.
This is also a good place to set the compliance boundary clearly. GaitExo acts as the trading and branding partner. We do not manufacture the devices ourselves. Our manufacturing partners include EULON (优龙机器人). GaitExo products are not currently CE marked as medical devices under EU MDR. The importer or distributor remains the local responsible party for medical device registration decisions. Our team supports documentation planning, export process clarity, and HS 8479.89 classification strategy where relevant.
How Can You Integrate Hip Assist Into an Existing Rehab Pathway?
A good device still fails if the team cannot place it inside daily care. Integration matters more than novelty.
To integrate hip assist into an existing rehab pathway, define the transition-phase patient group first, assign clear therapist criteria, and place the device between intensive gait training and discharge planning. Start with one workflow, then expand.
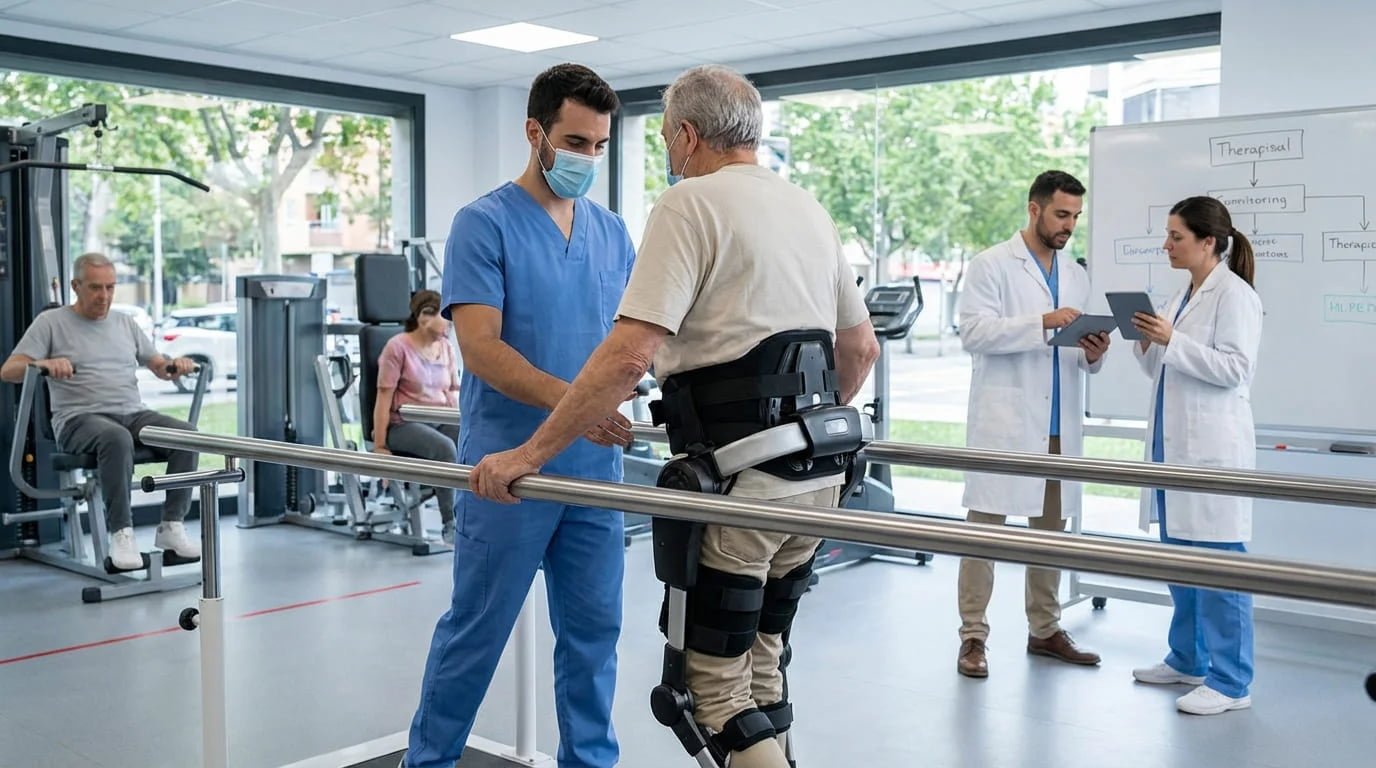
I usually recommend a simple rollout plan.
Step 1: Define one use case
Start with one target profile, such as post-stroke patients who have completed high-support gait training and now need supervised corridor walking support.
Step 2: Train a small therapist group
A focused therapist team creates cleaner feedback than a wide launch on day one.
Step 3: Set progression rules
Decide when the patient starts hip assist, what walking tasks matter, and when the patient exits the device pathway.
Step 4: Connect it to discharge planning
The device should not sit alone as a novelty item. It should support the move toward practical mobility goals.
Why this matters for hospitals and distributors
For hospitals, integration protects equipment use rates. For distributors, integration supports real adoption and repeat orders. That is one reason our team does not only discuss product features. We also discuss pathway design, package structure, and launch logic.
At GaitExo, we support a complete lower-limb portfolio across Gait Training Exoskeleton, Hip Assist Exoskeleton, and Ankle Assist & AFO Solutions. Standard lead time is 4–8 weeks from order confirmation. We usually work on FOB or CIF terms and provide full English technical documentation, user manuals, and remote support. Exact pricing depends on configuration and volume.
Hip exoskeletons can fill the transition gap that many rehab pathways miss. When the category is used well, it helps connect structured training to practical walking progression.




